What happens in the hearing test?
A thorough hearing test will have a number of steps. Not all are required for every person, but it’s worth knowing what to expect when you go to a clinic, to ensure you are prepared, and to make sure you get the required service. Ultimately, your Hearing Healthcare Professional (HHP) wants to find out how they can help you so a thorough hearing test should be expected, to get all the relevant information.

Case history
This is generally the first part of the hearing test. Some Hearing Clinics get you to fill in a case history form in the waiting room prior to your hearing test. In other clinics your HHP will ask you a series of questions about your hearing health (previous ear infections or ear surgery), your medical history (any major illnesses or medications you’re taking), family history of hearing loss, any exposure to loud noise (work, recreational or military service) and the situations where you’re having communication difficulties.
They will then look in your ears with an otoscope to check for any anomalies and if your ear canals are clear of wax. If wax removal is required, they’ll let you know. Your clinician may have the necessary skills to remove the ear wax, or they may refer you back to your GP to get the wax removed. If you know you have issues with wax build up, it’s wise to get this attended to prior to coming in for your hearing test as this can save you a lot of time.

Steps in the hearing test – what should be carried out?
Generally your Audiologist or Audiometrist will carry out three parts of a hearing test:
- Middle ear function test (not all clinics do this) – this is a relatively quick test where a probe is placed in the entrance to your ear canal and you will feel a pressure change in your ears as the tympanometer measures the mobility of your middle ear system. You may also hear some quite loud beeps during this assessment. Please note, that this is not a test of your hearing and you don’t have to respond in any way. You’ll be advised to keep still and not to swallow during this test.
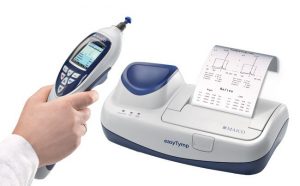
- Audiometry assessment – at this stage you may be asked to step into a sound proof booth (not all clinics have one). If you’re claustrophobic, let your clinician know and they will leave the door open for you. Headphones or insert earphones will first be placed over/in your ears – the clinician is testing your hearing via air conduction in this part. You’ll be given a response button to press when you hear a tone, no matter how soft. You’re being assessed for your threshold of hearing, that is, where you just hear a sound so it’s important to press the button even if you’re not sure you heard it. You’ll hear different frequencies of sound and each ear will be tested separately. Once this part is finished, the headphones/insert earphones will be removed and a bone conductor placed on your head. You are now being assessed for bone conduction. The bone conductor is a tight headband with a black vibrating box which is placed behind your ear. The sounds from this instrument can be heard anywhere in your head – it doesn’t matter where you hear it, still respond by pressing the button. Depending on your hearing levels, the clinician may also need to carry out masking in the audiometry assessment. This is a little more complicated and involves whooshing-type sounds being sent to one ear, while you listen for beeps in the other ear. Not everyone requires this part of the test.
- Speech testing – this is a test where you’ll listen to single words and repeat them back. The words will be at a few different levels – easy to hear, louder and softer. The clinician records your responses. Your hearing test is now complete.
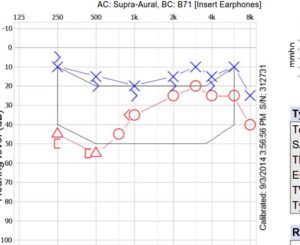
Getting the results
This is an important part of the appointment where your results are discussed and recommendations provided by your HHP. Your clinician should explain your hearing results (the audiogram) clearly and explain how your hearing levels are affecting your communication. Ask for a copy of your audiogram. The following options should be discussed:
- If your hearing is normal, come back for a retest every 12 months (just like you do with your vision test)
- If you have a medical issue with your ears you’ll be referred to your doctor
- If you have a hearing loss that can’t be medically treated, a hearing device will be recommended.
Next Article –> Questions To Ask
Previous Article –> Your Hearing And Lifestyle Needs
